Animals Aging Well
For the nation’s 40 million elderly pets, advances in veterinary care ensure the twilight years can be good ones
By Catherine O’Neill Grace
When Stefano Pizzirani, a veterinary ophthalmologist, examined Rocky, a 15½-year-old Standard Poodle, the dog was blind. White, dense cataracts clouded the lenses of both eyes. During a pre-operative workup for cataract surgery at the Foster Hospital for Small Animals at Tufts, a chest X-ray revealed small metastatic masses in the poodle’s lungs. Was the eye operation advisable?
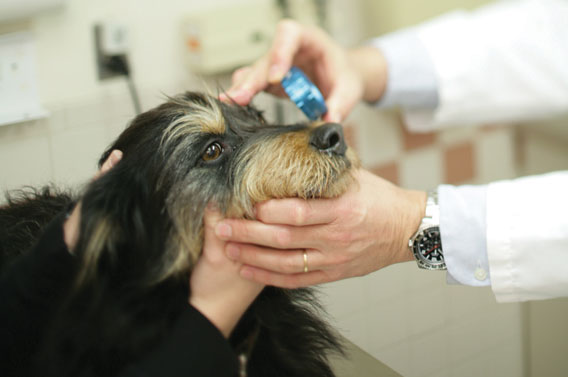
An older dog undergoes an eye examination at the Cummings School of Veterinary Medicine. Companion animals are living longer, thanks to advances in medical treatment and care. Photo: Steven Vote
“We discussed with the owner how appropriate it would be to do the surgery,” says Pizzirani, an assistant professor at the Cummings School of Veterinary Medicine. “The masses were small and were not causing any problems at that point, but they would progress. The owner said that the dog was young-behaving and very happy to play outside, but his blindness had caused some depression. ‘I want to offer my dog the best quality of life for whatever time he has left to live,’ the owner told us.”
The morning after the cataract surgery, Rocky was able to see and was soon chasing after his toys. “The dog was active, alert and very, very joyful,” says Pizzirani.
Rocky lived another year after the surgery. “His owner was so pleased about the results,” Pizzirani says. “Rocky was an old animal with lung cancer, and common sense would have suggested not doing his eye surgery—but he lived one more year, happy to play outside and to see again.”
Aging animals like Rocky comprise more than a quarter of the U.S. pet population, according to the American Veterinary Medical Association, which reports that 28 percent of dogs and 25 percent of cats are at least eight years old— a common benchmark for classifying an animal as a senior citizen. The most recent pet population statistics from an American Pet Products Manufacturers Association survey in 2007–08 reported 74.8 million dogs and 88.3 million cats in U.S. households.
Using a rough definition of “senior” status, that means that more than 40 million pets in the U.S. are elderly right now— or getting there. Older pets suffer from many of the same ailments as aging humans—failing vision and hearing, heart problems, arthritis and cancer. And the prescription for living well in those sunset years is remarkably similar: a healthy diet, moderate exercise and regular medical care.
How Old Is Old?
The definition of a senior pet varies widely, depending on species and breed. The old saw that one human year equals seven dog years is just that—urban legend. Even the American Animal Hospital Association’s (AAHA) senior care guidelines, published in 2005, are not definitive. The AAHA recommends that dogs and cats should get senior wellness screening exams starting at age seven or eight, although large-breed dogs may reach that screening threshold a year or two earlier. Instead of trying to equate animal age with human age, the AAHA recommends “applying senior guidelines to animals that are in the last 25 percent of the predicted lifespan for their breed and species.”
For example, a Saint Bernard may be considered a senior citizen at age six, while medium-sized dogs usually don’t show signs of aging until they are between nine and eleven. Small breeds, such as toy poodles, probably won’t exhibit age-associated problems until they’re eleven or older. “A nine-year-old Great Dane is ancient; an eight-year-old mastiff is a very old dog,” says Lisa G. Barber, an oncologist at the Cummings School. “But an eight-year-old Chihuahua or Yorkie is a youngster.”
Most cats are considered old at seven to eleven years of age—but some live much longer. The average life expectancy of a cat has nearly doubled since 1930, according to the Humane Society of the United States, and indoor cats live an average of eight to sixteen years.
In aging animals, just like in humans, things simply start wearing out. Older people and animals suffer from vision changes, loss of hearing, dental problems, high blood pressure, heart disease, arthritis, kidney and thyroid problems and cancer. And, as a result of better medical treatments and care and healthier lifestyles, both are living longer.
“We are seeing a whole bunch of new problems because animals are living longer,” says Mary A. Labato, V83, head of small animal medicine at the Foster Hospital. “Diets are better, and more people are considering a pet a family member instead of just a barn cat or a backyard dog. People don’t [take their pets] to the vet just for a rabies shot. Now it’s yearly checkups—and a lot of people are willing, for animals that fall into the geriatric category, to get twice-a-year checkups when necessary. We are much better at pain management, which is another reason for longevity.”
In her 27 years at the Cummings School of Veterinary Medicine, Labato, a kidney specialist, has seen many success stories with her senior patients. One of her favorites was a cat named Annabelle.
“Annabelle lived to be twenty-three,” Labato says. “She had chronic kidney disease for the last five or six years of her life. She weighed only four pounds. She was a tiny little cat but with lots of spunk. Her owners brought her in for repeated urinary tract infections. We treated her kidney disease, gave her a special diet, controlled some blood pressure and heart problems that she had—and she did fantastically well.”
The most common ailment in older cats is hypertension, Pizzirani says, “and the eye is the target organ. We see cats with hypertension that are twelve, thirteen, fourteen years old.” He recommends annual exams for cats older than eight. “You can pick up the early changes that can make a real difference. We can prevent retinal detachment and blindness. It’s treatment for the quality of life—and that is the whole point.”
Older dogs also are susceptible to age-related eye problems, specifically opacity, or cloudiness of the lens, a condition that worries owners, he says. “It is not causing any problem in vision,” Pizzirani says. “The pupil may become grayish or whitish, but they can still see. This is what causes people over age forty to have to wear glasses—the lenses change shape. We think that dogs do not experience the problems that people do with far- and nearsightedness.” And besides, Pizzirani says, animals “don’t have to read.”
Arthritis is another age-associated ailment that dogs and cats share with humans. “We see dogs with bad knees, bad elbows and bad hips, as well as arthritis in the spine—they’re very similar to people,” says Randy Boudrieau, head of small animal surgery at the Cummings School. Hip replacement surgery is done routinely, and in March, Tufts veterinarians performed their first elbow replacement on a Labrador retriever.
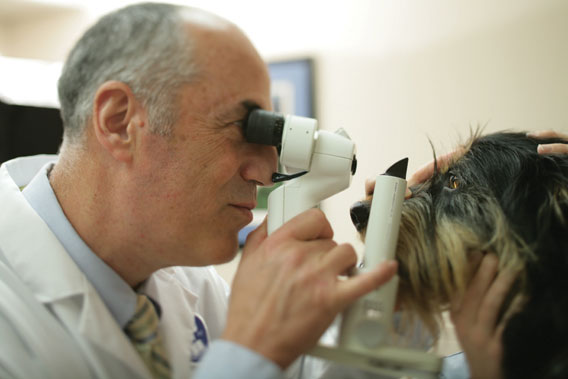
Ophthalmologist Stefano Pizzirani examines his canine patient for signs of age-related eye problems. Photo: Steven Vote
For older animals, the management of arthritis is similar to what physicians recommend for their human patients: control the weight and exercise in moderation. Boudrieau adds that there is a lot of evidence that overweight dogs’ arthritis will improve if they drop a few pounds. “We tell people if their dog is overweight you may have to back off and keep them on the slender side—no more table scraps.”
He also cautions owners against over-exercising their elderly animals.
“Dogs have no common sense,” he says. “If they are outside having fun and see a squirrel, they will run after it. If they are playing with your kids, they won’t stop for a break. And like you after you shovel the driveway, they will have a flare-up the next morning. They slow down, but they don’t recognize that they’re slower, so you have to do it for them.”
Eating for Health
Weight control and good nutrition are critical for maintaining an aging pet’s health and preventing or minimizing disease, says Lisa Freeman, J86, V91, N96, a veterinary nutritionist. Many owners ask her about feeding their pets one of the many “senior” diets on the market.
“There is no one best diet for every older animal,” she says. “Just because a pet turns seven or ten or even thirteen doesn’t necessarily mean it’s old. Just because a food is marketed for older animals doesn’t mean it’s right for every older dog or cat.”
Individual differences aside, there are a number of changes that occur with aging that can affect nutritional requirements. Little research has been done on the dietary needs of aging companion animals, Freeman says, although dietary adjustments may help improve the symptoms or even slow the progression of diseases such as arthritis, hypertension and cancer.
“Many of our assumptions are based on research in other species in which digestion and absorption of nutrients can be impaired with aging,” Freeman says. “Dogs tend to have decreased energy requirements, decreased activity and gain fat and lose muscle. Immune function and kidney function also decline with age, although the degree to which this occurs depends on the individual animal,” she notes. There needs to be more research to determine “the optimal nutritional levels required by older dogs and cats.”
Many older dogs and cats do very well by continuing to eat a good quality commercial diet designed for adult pets. Others will benefit from a “senior” diet. “It is important to understand that there is no legal definition for ‘senior’ or ‘geriatric’ foods,” says Freeman, although such products generally contain less protein and phosphorus and fewer calories.
The bottom line in deciding what to feed an older pet, Freeman says, is the animal’s overall health. For cats with diabetes, for example, increasing fiber or using a high-protein, low-carbohydrate food may help to control the disease and reduce the need for insulin. A low-salt diet may help dogs with advanced congestive heart failure.
Living with Cancer
In animals, as in humans, cancer is another disease of old age. “We think of it as being the cumulative result of repeated assaults on an animal’s DNA over the years,” says Lisa Barber, the veterinary oncologist. Lymphoma is the most common cancer she sees in older dogs. Osteosarcoma, or bone cancer, is prevalent in large-breed dogs.
“Cats get cancer less often than dogs do,” says Barber, “but when they do, as a rule of thumb, it tends to be a more malignant disease.”
While some animal cancers can be discovered during a general physical exam, cancers that occur internally are not easy to recognize and tend to be diagnosed after they have started to cause other problems—for instance, when a tumor pushes on a dog’s intestines and causes gastric symptoms.
“What’s unfortunate about internal tumors is that they are often diagnosed at the later stages,” Barber says, “but that does not mean that it’s hopeless. For instance, if there’s a tumor that’s pressing on the intestines and stopping the flow of food, that animal could be very sick. And yet if the tumor is amenable to surgery, the animal can do very well afterward.”
The treatment of animal cancers mirrors that for malignancies in humans: surgery, radiation or chemotherapy—or a combination of them. When dogs undergo chemotherapy, Barber says, “they often do better than their owners would. We’re very fortunate in our veterinary patients, particularly dogs, that they don’t seem to get the same gastrointestinal side effects” as people undergoing chemotherapy do.
For an owner of a pet with cancer, the ability to have more time with a beloved companion is indeed a gift. “I enjoy every minute with Zeus as he responds so well to his chemotherapy and acts like a three-year-old—not a fourteen-year-old, cancer-afflicted cat,” wrote Agnes Varis, H03, a Tufts University trustee and overseer to the Cummings School. To help other animal owners afford the cost of cancer treatment, Varis, a longtime benefactor of the Cummings School, established the Zeus Varis Fund.
“People think of cancer as a hopeless disease, but it does not have to be,” says Barber, who consulted about Zeus. She remembers a dog she worked with during her early training. “The dog had relapsed lymphoma and came in very sick. It was treated with a new drug, and I had to go to the owner’s house to deliver some paperwork about it. It turned out to be an important moment in my career,” she says. “The dog was out in the backyard running around. The owner thought it was a miracle. She said, ‘You have to feel the lymph nodes; they’re so much smaller.’ I did, and I couldn’t believe it was the same dog thirty-six hours later.
“We can help animals,” Barber says. “This is a field that is growing and expanding in terms of therapeutic options. Of course it is heartbreaking at the end—and that is true of heart disease or kidney disease or any other illness. But in between the diagnosis and the end, there are many pets that can live very happily—even if only for a year. And that year is precious.”
This story first appeared in the Spring 2009 issue of Tufts Veterinary Medicine magazine.
Catherine O’Neill Grace can be reached at catherine.grace@tufts.edu.

